Dr. Alfredo Ribeiro-da-Silva, McGill University, is a serial publisher of studies using our
pain and inflammation research antibodies.
Here, use of our
rabbit anti-CGRP and
guinea pig anti-P2X3 is referenced. Please note the high titer of these antibodies (dilution is 1:25,000):
Abeer W Saeed, Alfredo Ribeiro-da-Silva. Non-peptidergic primary afferents are presynaptic to neurokinin-1 receptor immunoreactive lamina I projection neurons in rat spinal cord. Molecular Pain 2012, 8:64 doi:10.1186/1744-8069-8-64.
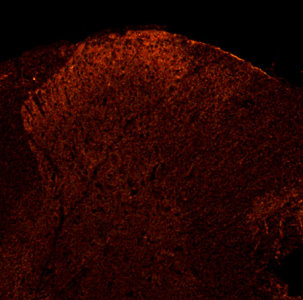
Images: CGRP, IB4 and P2X3 staining in transverse spinal cord sections. A and B show low magnification confocal images of CGRP-IR and IB4 positive (A) or P2X3-IR (B) fibers. C and D represent high magnification confocal images from the middle third of the lateromedial extent of the superficial dorsal horn. In C, note that there is limited co-localization of IB4 and CGRP (in yellow). Arrowheads show axonal varicosities (boutons) from nonpeptidergic fibers in lamina I, which do not co-localize CGRP immunoreactivity. The framed regions in A and B indicate the approximate regions from where C and D, respectively, were obtained (the latter originate from other sections). CGRP (in green); IB4 (in red); P2X3 (in red). Scale bar (A, B) = 200 μm; scale bar (C, D) = 20 μm
Tissue processing: The injection site at the level of the parabrachial nucleus was examined by cutting serial, 100 μm-thick coronal sections of the relevant brain region. The dorsal aspect of the L4-L5 spinal cord segment was cut into serial, 50 μm-thick horizontal sections (n = 10), 50 μm-thick parasagittal sections (n = 4) or 50 μm-thick transverse sections (n = 4). All sections were cut using a freezing sledge microtome (Leica, Richmond Hill, Ontario) and collected as freefloating in phosphate-buffered saline (PBS) with 0.2% Triton-X 100 (PBS + T). To block unspecific staining, all spinal cord sections were incubated, for one hour, in 10% normal donkey serum (NDS) (Jackson, West Grove, PA) in PBS + T at room temperature. Subsequently, the sections were placed in primary antibodies (or conjugated lectin IB4 - see below) for 48 hours at 4 °C. We used a mixture of 2 or 4 primary antibodies (each raised in a different species), or IB4, in PBS + T containing 5% NDS. Next, the sections were washed in PBS + T and then incubated in species-specific secondary antibodies that were raised in donkey and conjugated to either AlexaFluor 488, AlexaFluor 405, Rhodamine RedX or biotin. The sections were incubated in 3 different cocktails: #1) rabbit anti-CGRP at a 1:200 dilution (Sigma, St Louis, MO) and lectin IB4 conjugated to AlexaFluor 568 at a 1:200 dilution (Molecular Probes); #2)
rabbit anti-CGRP and guinea pig anti-P2X3 at a 1:25,000 dilution (Neuromics, Edina, MN); #3) goat anti-CTb at a 1:5000 dilution (List Biological), rabbit anti-NK-1r at a 1:10000 dilution (Sigma, St Louis, MO), guinea pig anti-CGRP at a 1:8000 dilution (Peninsula, San Carlos, CA) and lectin IB4 conjugated to AlexaFluor 647 at a 1:200 dilution (Molecular Probes). All the sections were washed with PBS + T and then (for #1) incubated for 2 hours at room temperature with donkey anti-rabbit AlexaFluor 488; (for #2) incubated for 90 minutes in a biotin conjugated donkey anti-guinea pig IgG (Jackson Immunoresearch, West Grove, PA, 1:200). Further signal amplification was achieved by treating the sections with 1 hour incubation in an avidin-biotin (A + B) complex (Vectastain Elite ABC kit, Vector Laboratories) followed by tyramide (Perkin-Elmer, Norwalk, CT, 1:75) for 7 minutes. Sections were then incubated in streptavidin conjugated to AlexaFluor 568 (Molecular Probes, Eugene, OR, 1:200) and donkey anti-rabbit AlexaFluor 488; or (for #3) incubated for 2 hours at room temperature with secondary antibodies: donkey anti-goat Rhodamine Red X, donkey anti-rabbit AlexaFluor 488, and donkey anti-guinea pig AlexaFluor 405. Finally, sections were washed with PBS, mounted on gelatin-subbed slides and coverslipped with an anti-fading mounting medium (Aqua Polymount; Polysciences, Warrington, PA). Slides were stored at −4 °C pending further processing.
I will continue to publish outstanding customer data/images using our natibodies/markers.